How point of care testing in the home is transforming healthcare
10 Nov 2021
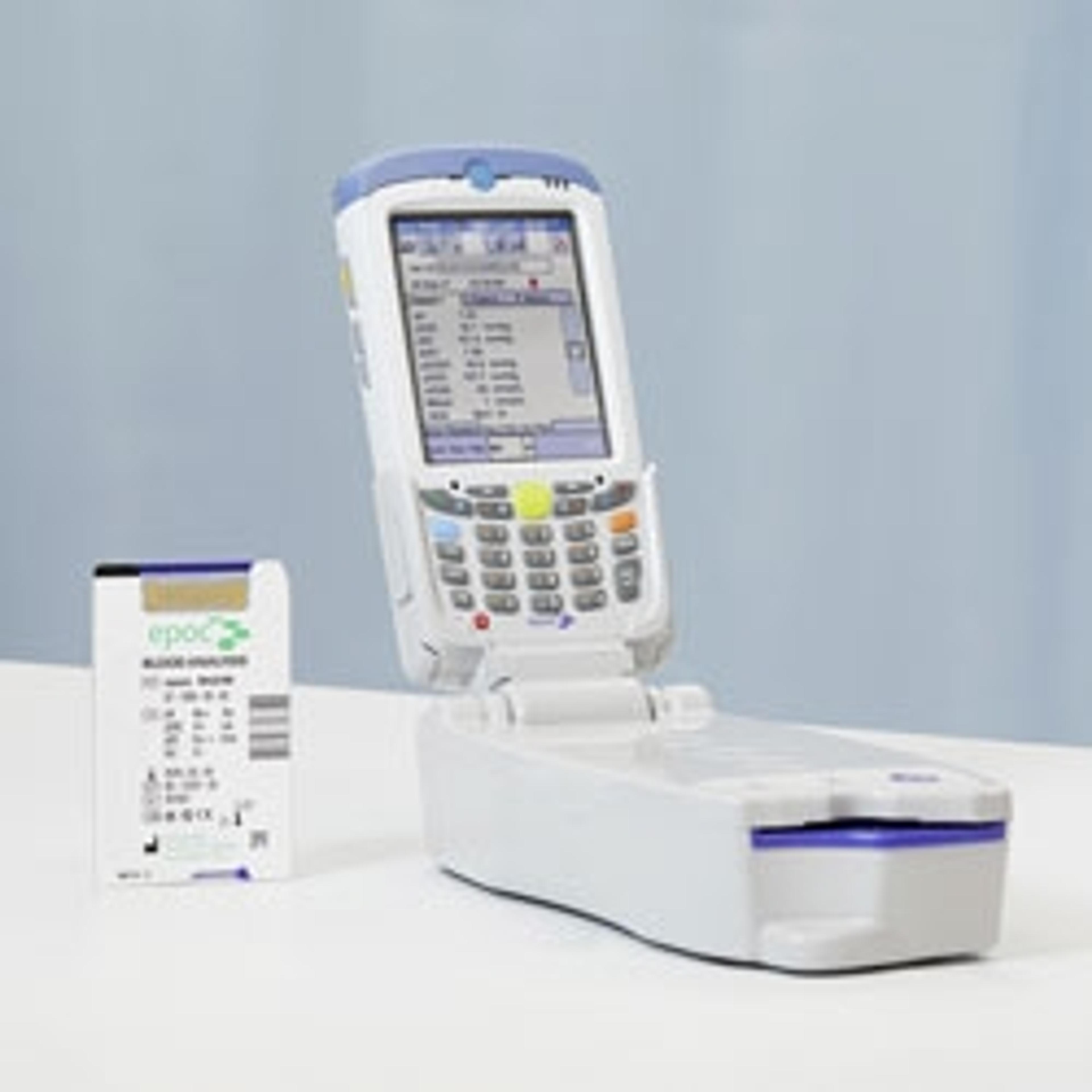
As Niagara Emergency Medical Services’ mobile integrated health program specialist for community medicine, Ken Kohut works with patients that are frequent users of emergency medical services. In this video, he explains how point of care testing, including blood analysis, performed in the patients’ own homes provides quantitative results that enable appropriate treatment decisions to be made that will in turn help to decrease unnecessary visits to hospital emergency departments or expedite emergency care where it is required.